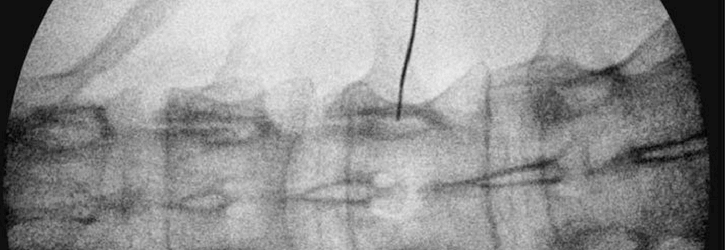
For the treatment of CRPS, sympathetic nerve blocks are a standard weapon in the arsenal of the specialist pain doctor.
What exactly are nerve blocks?
Sympathetic nerve blocks are injections of local anaesthetic and (often but not always) another drug to prolong the effect of the nerve block beyond the life of the local anaesthetic. Depending upon whether the CRPS has manifested itself in a lower or upper limb, the injection will either be administered into the sympathetic nerves in the lower back (a Lumbar Sympathetic Block) or into the sympathetic nerves of the neck (a Stellate Ganglion Block). The injection is administered under x-ray or ultrasound guidance in order to ensure that the medication is delivered to exactly the right spot.
The block targets the sympathetic nervous system which encompasses a series of nerves that spread out from your spine to your body to help control a variety of involuntary bodily functions, for example blood flow and sweating. It is thought that dysfunction of the sympathetic nervous system following trauma may play a role in the development of CRPS.
As specialists, we understand CRPS. Speak today, informally and in complete confidence, to one of our specialist solicitors on 01225 462871 or email us. We are confident you will notice an immediate difference and a very different service from your current solicitors. |
Nerve blocks serve two purposes: diagnosis and treatment
If the nerve block is successful in reducing the symptoms of CRPS, even for a very short time, that can suggest that there is damage to the sympathetic nerve chain and therefore help to confirm the diagnosis of CRPS. Blocks are not used as the only diagnostic tool and the failure of the block does not mean that the person does not have CRPS.
From a treatment perspective, it is hoped that a nerve block can stop the progression of CRPS or even reverse it, resulting in the CRPS going into remission. It should quickly become apparent if the block has been effective as the affected limb will start to turn warm as blood flow returns and pain relief should follow swiftly. If successful, the patient may be offered further blocks which it is hoped will provide successively more pain relief.
Are there any risks?
In addition to the more usual risks with injections such as the needle causing nerve damage or failing to inject the drug into the correct place, any injection for somebody suffering CRPS carries risks, primarily of causing the spread of the condition and it is vital that the necessary protocols are followed.
If the nerve block is carried out properly, other than the pain and discomfort of the block itself, for most people there are no adverse effects.
How effective are they?
To be honest, over many years of acting for people suffering CRPS, I cannot recall any of them reporting a significant improvement in their symptoms following a nerve block. A couple of people have reported some modest, short term benefit but, for different reasons, did not undergo repeat blocks.
However, despite my own experience, it is clear that sympathetic nerve blocks can and do work for a some people. Specialist pain doctors have contact with substantially more people with CRPS than I, and if they were not experiencing at least some degree of success then clearly (one would hope!) they would not continue to offer the treatment. There are also plenty of accounts online of people having a positive experience with nerve blocks, although most of them seem to have had their block very soon following the onset of symptoms.
Indeed, research has concluded that the duration between the onset of the symptoms of CRPS and the patient undergoing the nerve block is a significant determining factor in the prospect of success. As a very rough rule of thumb, it seems that a block has the best prospect of success if carried out within six months of the onset of symptoms. In fact, the earlier the better.
For many people, however, by the time nerve blocks are attempted, their CRPS may simply be too well established for the block to be effective.
You may also be interested in the following articles:
CRPS and Surgery – Unhappy Bed Fellows
Can Pain Pumps be effective for CRPS?
Who is likely to develop CRPS?
Hushed up? Could a simple antibiotic successfully treat therapy-resistant CRPS?